Hair loss is a common concern among men, but the biological causes behind it can vary widely. Because hair thinning may develop gradually or appear suddenly, understanding the nature of the change is important before drawing conclusions about its cause.
Medical doctors approach hair loss by examining several aspects of hair growth and scalp health. The goal is not simply to observe where hair appears thinner, but to understand what is happening at the level of the hair follicle and the hair growth cycle.
Careful clinical evaluation allows physicians to distinguish between different types of hair loss and to understand the underlying biological process affecting the follicles.
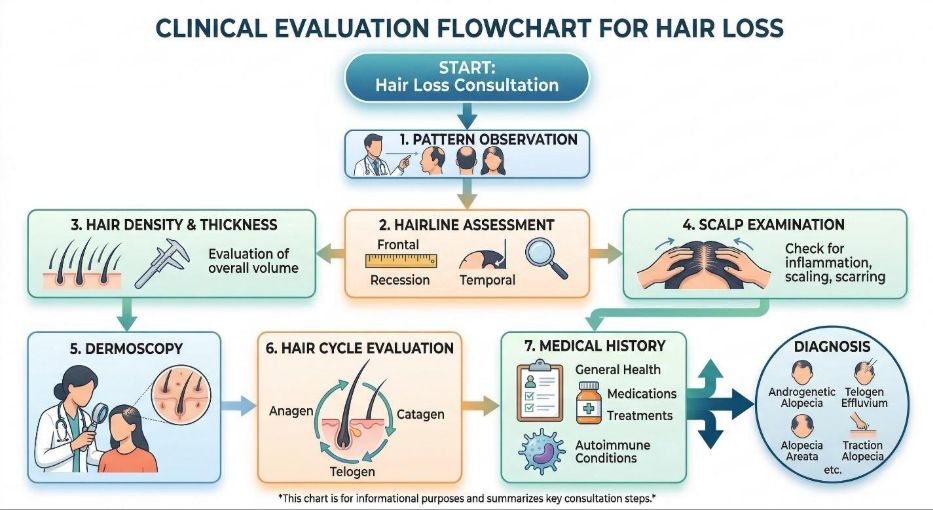
Observing the pattern of hair loss
One of the first steps in evaluating hair loss is to observe the pattern of thinning across the scalp.
Different conditions affect different areas of the scalp. In many men, gradual thinning begins at the temples or the crown and progresses over time. This distribution often reflects androgenetic alopecia, the most common form of hair thinning.
Other patterns may suggest different causes. Diffuse thinning across the entire scalp may reflect a disturbance in the hair growth cycle. Patchy areas of hair loss may indicate immune activity affecting the follicles.
Because the distribution of hair thinning often provides important clues, the pattern of hair loss is a key part of clinical evaluation.
Assessing the hairline
Changes in the hairline are often among the earliest signs noticed by patients.
Medical doctors examine whether the hairline has shifted backward at the temples or across the forehead and whether the density of hair along the hairline has changed. Subtle reductions in hair thickness may indicate early follicle miniaturisation.
The shape of the hairline also provides useful information. A mature hairline may remain stable for many years, whereas progressive recession may suggest an ongoing process affecting the follicles.
Careful observation of the hairline therefore helps place visible changes in context.
Examining hair density and thickness
Hair density refers to the number of hairs present in a given area of the scalp, while hair thickness refers to the diameter of individual hair strands.
Both factors influence how full or dense the hair appears.
during examination, medical doctors may compare different regions of the scalp to determine whether certain areas contain fewer hairs or whether the hairs themselves have become finer.
Because follicle miniaturisation produces progressively thinner hairs, changes in hair diameter can provide important evidence of underlying biological processes affecting the follicle.
The scalp examination
The scalp itself is also examined carefully.
Healthy scalp skin usually appears smooth and free of inflammation. In some conditions, however, the scalp may show redness, scaling, or other signs of irritation.
These changes may indicate inflammatory conditions of the scalp that can affect hair follicles.
Examining the scalp therefore helps determine whether hair loss reflects changes within the follicle itself or whether the surrounding skin may also be involved.
Dermoscopy
Medical doctors often use a technique called dermoscopy to examine the scalp more closely.
Dermoscopy involves the use of a magnifying device that allows the physician to visualise individual hair follicles and hair shafts at higher magnification.
Through dermoscopy, it becomes possible to observe differences in hair thickness, the presence of miniaturised hairs, and the condition of the follicular openings in the scalp.
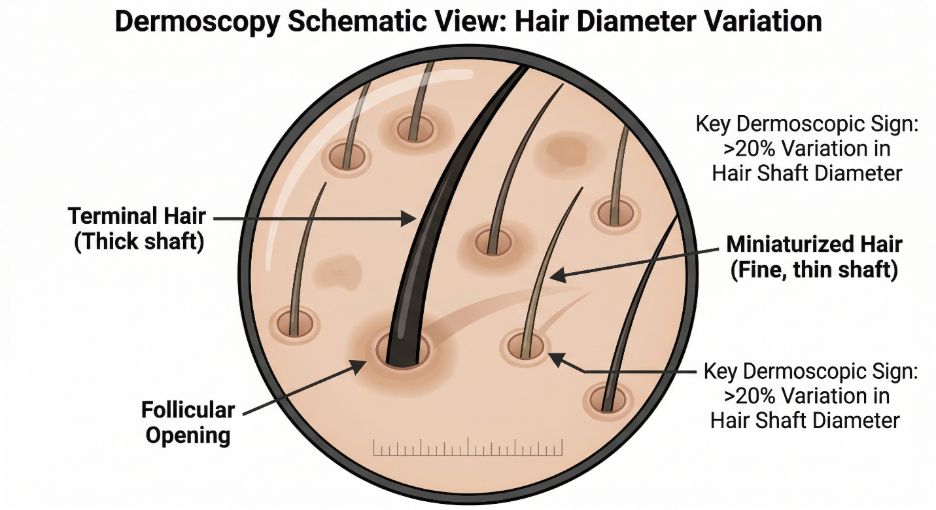
This tool can reveal subtle changes that may not be visible during routine visual examination.
Evaluating the hair growth cycle
Hair follicles move through cycles of growth, transition, and rest. When evaluating hair loss, medical doctors may consider whether these cycles appear to be functioning normally.
In some conditions, a larger number of follicles may enter the resting phase of the cycle simultaneously. This can lead to increased hair shedding several months later.
Understanding how the hair cycle is behaving helps explain whether hair thinning reflects gradual follicle changes or a temporary shift in the rhythm of the hair growth cycle.
Medical history and timing of hair changes
Hair loss rarely occurs in isolation from the rest of the body's physiology.
During evaluation, medical doctors often consider the timing of hair changes in relation to recent illness, major stress, surgery, or significant changes in general health. Because the hair growth cycle unfolds over months, events affecting the body may influence hair shedding after a delay.
Exposure to chemicals or medications is another important part of the medical history. Certain drugs, including some anticoagulants, antihypertensive agents, retinoids, and hormonal treatments, are known to affect the hair cycle and can cause diffuse shedding. Occupational or environmental exposure to chemical agents may similarly disrupt follicle function. Establishing whether such exposures coincide with the onset of hair changes is an essential step in clinical evaluation.
Autoimmune conditions are also relevant to a thorough medical history. In conditions such as alopecia areata, the immune system mistakenly targets hair follicles, leading to patchy or more extensive hair loss. Other systemic autoimmune diseases, including lupus and thyroid disorders, can also affect hair growth. Identifying whether an autoimmune process may be contributing to hair loss is an important part of a medically rigorous evaluation.
Understanding when the hair changes began, and in what medical context, can therefore provide valuable context for interpreting the pattern of hair loss.
Distinguishing between different causes
The combination of scalp examination, pattern recognition, and understanding of the hair growth cycle allows medical doctors to distinguish between different types of hair loss.
Gradual thinning at the temples and crown may suggest androgenetic alopecia. Diffuse shedding across the scalp may reflect a temporary disruption of the hair cycle. Patchy areas of hair loss may indicate immune activity affecting the follicle.
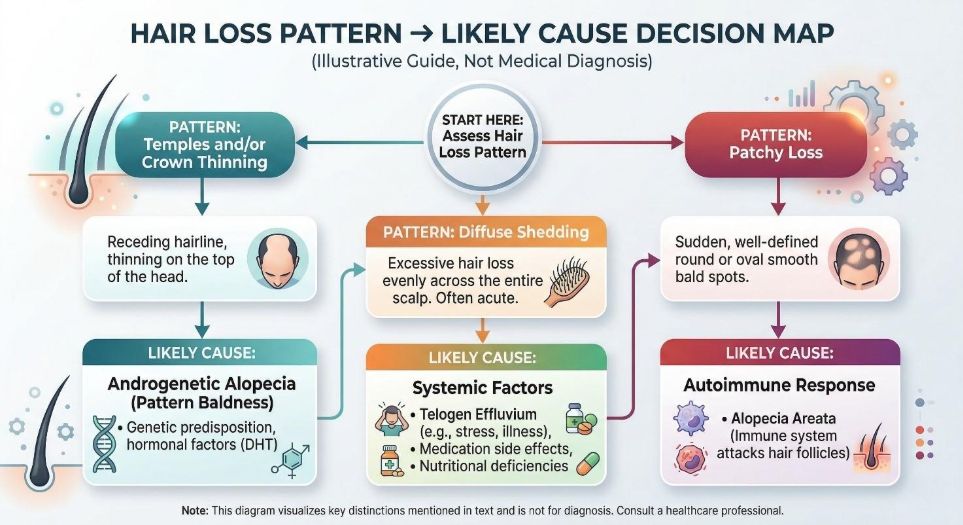
Each of these conditions affects hair growth through different biological mechanisms.
A clinical approach to hair loss
Evaluating hair loss involves more than simply observing the amount of hair present on the scalp. It requires understanding how hair follicles behave, how the hair growth cycle functions, and how different biological processes can influence both.
Through careful examination of the scalp, the hair shafts, and the pattern of thinning, medical doctors can gain insight into the underlying processes affecting hair growth.
This clinical perspective helps place visible hair changes within the broader biology of the hair follicle and the scalp.
Author: Dr. Priya Goswami
Medical review: Dr. Denis Broun
Next step
If you notice coverage changes without increased shedding, confirm what process is occurring.
Take the Hair Assessment to have a physician review your pattern, identify whether miniaturization is present, and determine appropriate staging and next steps.



Add Comment